So, I was going to break this into several entries...but the experience really melded into what felt like one long day...so I decided to keep it as one long entry. So, here you have my surgery day, and the 4 day hospital stay that went with it.
Surgery day, YIKES.
We woke up around 4:30 so that each of us could shower and be ready for the 6:00 departure.
My mom met us at our house around 5:45, and Dad-in-law met us at the hospital for 6:20.
When I first went in, I had to go to two different places to check-in and fill out lots of paper work. It moved relatively quickly, which was great for me because I hate lingering. I went into the surgery prep area around 7:30 where I had to get into my surgical outfit, a johnny and a new blue shower cap looking hat, woohoo. Once I was all suited up, a couple doctors/nurses came in to speak with and introduce themselves. They were my surgical nurses and some of my aneasthesiologists, very nice and caring. Almost right away, Dr. S came in to see me and had a nice long, calm conversation about the plan, and how he's hoping the day would go. The plan was as follows: Go in and get to the hip first. Then to assess the actual structure of the hip and begin cutting and placing bones as needed. Once they made one of the final cuts, he was going to decide if he wanted to look into the joint and see if he could tidy up the labrum a bit. If the labrum was accessible, an easy fix, and the rest of the surgery was going smoothly, then he would address the labrum while he's in there.
With all that being said, the aneasthesiologists started me on a IV of some wonderful things to "take the edge off." And it really did. Phew. We waited for just a few more minutes, and then I was off to the races. I said my goodbyes to my mom and my hubby (who were in surgical prep with me), and they wheeled me away.
Right before we left the surgical prep area, they gave me another hit of something else to help me relax while waiting for anesthesia. Don't know what it was, they didn't tell me...but boy oh boy, I had not a care in the world! I was thinking: "Allllllrrriiiigggghhhhtttt, surgery!"
I don't remember too, too much after that...but I do remember a couple glimpses of the operating room. Believe you me, they look NOTHING like they look on Grey's Anatomy. They are somewhat small, cramped with TONS of high storage systems with drawers, everything's covered in plastic and all you can see really are small passage ways to different machines/equipment. It was nuts. The last thing I remember is seeing Dr. Schiller in his surgical gear standing at the x-ray machine showing a group of Residents (I assume), the game plan for cutting the bone. Then in about a milli-second, the anesthesiologist put the mask on my face and I was O-U-T.
About five seconds later (real time approximately 6 hours), I woke up in recovery feeling VILE. Oh my gosh I can't even begin to explain the feelings. Easiest way to describe it is the world's WORST, most TERRIBLE hangover. It was like I had been trampled by elephants. I couldn't wake up for life of me, I lost so much blood in surgery my skin tone was a lovely mint color, and I was dry heaving every 2-3 seconds. It took me almost 2 hours and a blood transfusion in recovery to start feeling a bit more human. I honestly can't remember much hip pain, probably because I was so anxious about everything else. My recovery nurse, Sarah, was AMAZING. She helped me through the whole thing and stayed by my side the whole time.
Here's a glimpse into the surgery: It took longer than Dr. S had hoped (for whatever reason...not totally sure), and I bled more/faster than they were expecting. The combination of the two led to me losing about 1,600 cc's of blood. That's almost 2 LITERS. Now, mind you, they had the cell saver on, so they tried to recover as much as they could...but by the end of the surgery I really had lost a lot. More than anyone was really expecting. But, that's the thing, you can run every test in the world...but every person is different and bleeds differently. I don't blame anyone for that. You can't plan it, no matter how hard you try.
So...after that kind of blood-loss, your blood pressure PLUMMETS. I could see the read-out screen in recovery...and maybe I'm too smart for my own good, but I knew the heart rate and blood pressure numbers it was reading were really low. I was really tachycardic during and after surgery (had a very fast heart rate, almost 140 beats per minute, normal is around 90), and my blood pressure was so low it was shocking to me. It was in the 60/30's early on when I was so "drunk" I could barely move. It's generally supposed to be around 110/70. It came up very slowly, but still stayed low until a couple days later.
However, besides all of that crap, I was honestly so unbelievably thirsty! My throat hurt a little from the breathing tube, and I couldn't wait to have a sip of ginger ale (drink of choice in hospitals, apparently). I drank almost 2 cups of ginger ale in recovery while waiting for my room. That was such a bad idea...but it tasted so refreshing on my mouth and lips and throat, it was almost heavenly.
Now...I wasn't worried that it might be life-threatening or anything like that. The care around me, and just Sarah's presence alone, made me feel like I was perfectly fine. You know what I was ACTUALLY worried about? My HUSBAND and family waiting for me to come out of recovery! I know my husband is a worry-wart, and I knew he was ticking down the minutes. The Dr. told him I'd be out of recovery in about an hour, at that time we were working on almost 2 hours until I was good enough to see him. When he came in, I looked a lot better (color wise), and I had become a bit more understandable with my language. I felt a lot better, and like I could relax when I saw him and he knew I was okay.
He waited with me until they brought me to my room. And then the whole family came with me as I entered my new home for the next four days. Of course, once you get in your new room, you have to do the hospital bed transfer...or otherwise known as the most humiliating thing in the world. They turn you and tug you and undress you and your catheter is uncomfortable and you're not feeling well from anesthesia and your roommate's family walks by and you moon them with all of your most private parts. SIGH. That was awful. Seriously. It took a couple minutes to get it right because of my hip...I couldn't have been more thankful when that was over...let me tell you.
So...I get settled in my bed, my family comes in and we sit. Well...they sit...and I sleep....sleeep sleeeppp, sleep. They went to get dinner, because I was so out of it anyway...it didn't matter. By the time they came back about an hour and half later, I was finally awake enough to spend time with them. Dr. S. came by too, which really made my night. He was so excited about the success of the surgery, he gave me great coverage, enough he thinks, to probably last me until I'm close to 70. That was really great news. I had already heard that from hubby, but it was nice to hear from the Doc himself. The other thing Dr. S. did tell me was that because of how long it took him to give me that fantastic coverage, they didn't have time to look at or address the labrum. This means that about 8 weeks from now, I will need to have follow-up surgery. Not the best news...but I'm so unbelievable happy with the success of the PAO, that I'm really not worried about the hip scoping!
Dr. S left for the night, and at that point...I had been having some pain in my hip...probably about a 6 out of 10. The lovely nurse decided to give me some dilaudid. And by some, I mean 2 mg. May not seem like a lot, but I am a teeny, tiny person...and dilaudid is synthetic morphine. So...2 mg sent me FLYING HIGH. What a strange feeling when they administer it! It was like a wave of heavy heat floating across my chest...so strange and unnerving...I really didn't like it. What I also didn't like, wass that about a millisecond after I was given the 2 mg...I felt like a stoner who couldn't talk, or communicate...or do anything except sleep. My hubby was actually worried about it, because I fell asleep/half conscious almost immediately.
And then came the sickness. Oooohhh boy...the sickness. I booted (puked, lost my lunch, praised the porcelain god, upchucked...you get the idea). I booted what felt like 100 times for the next three hours. Every ounce of anything in my body came out...and I just laid there like a beaten woman. It was AWFUL.
Around 8 o'clock, they started with my second blood transfusion. My blood pressure was still pretty low (for me), and they wanted to get it back up to normal. The blood they gave me for both transfusions was O-. Which was surprising to me because they had all the necessary info to give me MY blood type (A-). Why use the O- when you can use the correct kind? These things baffled me...and it turned out my baffled nature was instinctively correct. By 1 am, mostly through the transfusion, my temperature had risen to 100.8. That's a bad sign during a blood transfusion, because it means that your natural blood is not playing nice with the transfused blood. At this point we had to do all sorts of blood and pee tests to make sure my body wasn't freaking out completely. Once my transfusion was over, all we could do was just wait and see what happened.
My fever from the transfusion kept up in the low 100's to as high as 101.4 until around 2-3 am on Sunday. It finally broke and I started to feel better.
Saturday was an okay day, besides the fever mishap. Physical Therapy (PT) came and got me out of bed using a walker and in a reclining chair. Such a seemingly small thing, but it was a huge effort for me! I was so happy when I sat in the chair. Felt so good, empowering even.
I mostly just rested and visited with my mom and hubby after that. Slept when I wanted, watched TV, drugged up to ease the pain, and just vegged out. I started on real food that day...I mean...if you call hospital food "real." This day they also stopped the IV Dilaudid and started me on pills: Oxycodone.
Sunday was a good day, except for the morning. I had a BUSY morning, and it led to me feeling really nauseas. I had the catheter removed, I was told to get up using the walker and get out of bed and in the chair for breakfast, the Fellow came and pulled my incision drain out and changed my dressing, then I had breakfast...all within an hour and a half time frame. It was just way too much, too fast. I got really dizzy and nauseas and had to have some zophran for the nausea.
After a couple hours though, I was feeling much better...had a really good Sunday. I had hardly any pain to speak of. My blood pressure had come up and my fever had broken. I also had some good PT with the nurses where I got up and used the walker to walk to the bathroom by myself and back to the bed. Things were looking up. Dr. S came in (on his off day...mind you), to check in with me and see how I'm doing. Answered all of our questions, while his adorable little daughter waited out in the hall way. Dr. S was so happy with all of my progress, that he was saying I could go home the next day, if I wanted to! There was light at the end of the tunnel. But unfortunately...going home on Monday was not a good idea. Hurricane Sandy was going to strike that day...and they didn't want me traveling/going home with such treacherous conditions.
So...Monday came and went. Was a great day, my best day yet. I felt awesome (in an obviously relative way), hardly any pain at all. I wasn't on the pain meds much at this point...only (as instructed) before PT. I slept well, I ate well, and I went through some really good PT where I used the walker and walked all the way down the hallway and learned some exercises for my leg. It was nice to be doing so much!
Monday night I didn't sleep very well, I had a new roommate who was rude and inconsiderate of my needs. Won't go into details...but many times I fondly referred to her as "The Wench." I think I was also anxious because I knew I was getting out of that place. While the staff and everyone was SO great, I really wanted to get home and start the real road to recovery.
Tuesday came and went so fast. I had PT in the morning to see if I could pass my last tests before being discharged. The major test was stairs, to see if I could go up and down stairs with the crutches. I passed the test with flying colors. I did have breakfast and lunch in the hospital, which was nothing write home about...but it kept me occupied while I waited for all the discharge papers to come through. It took until 3 for everything to be settled for me to leave the hospital...I can't understand that! But...that's okay. I keep telling myself...I know a lot of people have to sign off on it...and everyone is very busy.
Anyway, the couple main things I took away from this surgery and hospital stay were as follows:
- I think they serve better foods to inmates.
- Nurses/CNA's are BUSY. Unbelievably busy. And while I appreciate every single thing they did for me...the one piece of advice I would give someone going into and extended hospital stay is this: the very SECOND you feel like you have to pee (or whatever), push that call button like it's going out of style. On average, I had to wait almost 15 minutes for someone to come help me go to the bathroom. And after I had the catheter taken out, I needed to pee really often. I couldn't get out of bed on my own (for obvious reasons). That may not seem like a super ridiculous period of time...but when you've just gone through a traumatic surgery...where they cut a series of muscles in your thigh and pelvis...you better believe that holding it is not your strong suit. There were several instances where I really thought I wasn't going to be able to hold it.
Lastly, and most importantly:
- The nurses and CNA's and the staff at Rhode Island Hospital are top notch. Unbelievably nice, helpful, knowledgable and extremely selfless. I was amazed, time and time again, at how caring they were, even to the cruelest patients. It takes an exceptionally caring person to be a nurse. Makes me even more proud that my brother went into that field.
- I am so THANKFUL to blood donors. I always knew it was important...of course...but it puts into a whole new perspective when you're staring at a unit of someone else's blood dripping into your body for your health, that someone so graciously donated to a stranger. Seems like such a small thing...but it really was a touching moment for me. Not to mention, I had to have 2 transfusions, so that's 2 different people who gave me a piece of them...not even knowing me. Really amazing stuff...if you ask me.
So, that is that! Please, please, please feel free to ask me any any all questions you may have. I had a great experience, overall...and would love to help anyone else preparing for this to understand the in's and out's of my journey.
Thanks so much for reading!
D
Thursday, November 1, 2012
1 Day until I go under the knife!
I’m writing this in past tense because the few days leading up to the surgery were just too crazy to blog at the time. I had to get a lot of things in order before the 26th, many of which were not actually surgery related...I’ll spare you all the details and just let you know what my last day on my bum hip was like.
I took the day off from work, and had a day all about me. I slept in late, had some Dunkin’ Coffee and a breakfast sandwich, and then went for a 90 minute massage.
The massage was the most amazing thing ever, EXACTLY what I needed. I’d never had a real one before, so I wasn’t sure what to expect. Let’s just say, it’s worth every single penny you pay.
After the massage, I went and got a pedicure. I hadn’t had one in an age and I kinda wanted the extra pampering. It was really nice to just sit back and be taken care of. Ahhhh, it was so relaxing.
When I left the salon, I came home and rotted on the couch while watching some junky TV, it was GLORIOUS. And after a couple hours of that, I changed into cooking/baking mode.
Hubby arrived home from work around 5, and found me BUZZING around the house. I couldn’t keep still. I had made a list of things I wanted to accomplish before the surgery, and I felt desperate to complete them. He had to stop me several times just to try and calm me down. I was so anxious and nervous that I didn’t want to sit still...or all I would do is think about the next day. That would make me crazy.
I ran around the house most of the night, baking cookies and finishing goodie bags for my nurses, making a couple meals for us to eat, and packing my bag for the hospital.
We finally went to bed around 11:30, but I don’t know if either of us really slept at all. We had to be at the hospital at 6:30 am the next day...and we were just so anxious to get things going and get it over with.
The moral of this day was to just relax and prepare, so that’s really all I did.
Read on for info on the actual surgery day.
Friday, October 19, 2012
7 Days!!!
T-7 days! Wow!
Time is just flying by and I can’t believe that we are now just one
week from surgery. I am getting (insert any number of emotions here). All sorts
of exciting things have happened, depending on what your idea of exciting is.
I’ve applied for my handicap plate, I’ve applied for short term disability and
temporary disability insurance, and I’ve even rented a wheelchair. I’ve started
preparing my house so that I can be downstairs the majority of the time and not
be bored out of my mind. I went for my pre-op blood-work (I’ll be sure to
report back my “coagulation time”, I’m sure you all want to know), and I’ve even
purchased all of the stuff for the goodie bags for my nurses. It’s important to
say “thank you” to them, I know it can be thankless work and I want to make
sure they know I appreciate all of their help. Plus it’s around Halloween and I
love putting together little things like that.
Right now, I am a busy little bee, so I’m sorry I haven’t been
keeping you up to speed. I’ve got a lot of Relay for Life things going on, and
I’m reallllyyy trying to keep up with my volunteering work at the zoo. It’s
been hard to juggle everything, and to be honest, the mileage I have left on
this hip is just so low. I can’t really do much of anything without the pain
cramping my style. It’s really exhausting to be in pain all the time…I am
looking forward to some relief! And quite honestly, I think I could use the
down time!
Speaking of relief, my mom-in-law recently got me in touch with a
girl who has had the same procedure that I am having! She is similar in age,
and has the same issues with DDH. For the purposes of her privacy, we’ll just
call her D. D had her surgery a few weeks ago. She said she was in the hospital
for about 5 days. She did say that it has been a really eye-opening experience
to see how little you are able to do post-surgery. She’s very independent (just
like me), and doesn’t like to not be able to do things (she sounds like another
me, I like her already!).
When D and I started e-mailing back and forth, I asked her about
what caught her off-guard, or what she wasn’t expecting. She told me that the
biggest things were that she was given an epidural for three days after the
surgery so she didn’t feel pain (I had never even thought of this), and that generally
speaking, she is not used to the crutches and the wheelchair. She did mention
that I should definitely practice using the crutches on the stairs before the
surgery to get the hang of it. So from now on, I’m putting the crutches by the
stairs and will use them to go up and down. I think hubby and I have decided
that I’m going to try and sleep downstairs for a little while until I’m
comfortable enough to try going upstairs. I don’t know how long that will be.
Either way, our bed is very high, so I won’t be able to sleep in it anyway.
I’ll be sleeping on the futon in the office for a while. The thing I’m most
concerned about is accidentally using the hip…I’m thinking the less I move
around, the better. Even if I’m on crutches, there’s no guaranteeing that I won’t
accidentally slip and step onto the leg…I don’t even want to take that chance for
a while. I’m going to have to be super careful.
D also said that I should do the physical therapy exercises every
time I’m supposed to regardless of how I’m feeling, because she thinks it might
help make a difference.
Mostly, it was just great to know that there is someone else
similar in age that is going through this. I often feel a bit like an odd-ball
because of my hip deformity. It’s nice
to know there’s someone I can talk to that understands what it’s like to have
this kind of pain and the limitations that come with it. The best news is she
said she is feeling so much better already! It’s only been a few weeks and she
said she’s feeling pretty good! That’s good news, and very reassuring. I’ll be
interested to hear how she’s feeling once she starts walking on it.
Today, my co-workers had a little surprise “get well soon” party
for me. It was a nice little surprise and really made me feel great. It’s nice
to know you’ve got such a great support system. I’m a very lucky girl.
Other than
that, my days have been filled with very random things, trying to finalize
everything as much as I can before next Friday. I’m working Monday-Wednesday,
and I’m taking a ME DAY on Thursday. I am going to get a massage, a manicure
and a pedicure, and probably do some last minute shopping for goodies while I’m
laid up. Friends have given me all sorts of gossip magazines, movies, etc…so I
think I’ll be just fine! I’m really getting restless, not sure what to do with
myself these days. This weekend I’m going on a camping trip with my mom to try
and spend some quality time with her before my surgery. That should be really
great, I’m looking forward to that.
Well, that’s it for now! I will check back with you next week
sometime, when I know what the surgery day is going to look like!
Thanks for reading,
-D
Thursday, August 23, 2012
9 weeks, 1 day
Well hello!
I know I was supposed to be back on here and write you all after
my surgery consult on August 6th, however (and I know this will be
surprising), that appointment was cancelled. He “wasn’t going to be able to
make it” that day, so we re-scheduled for August 20th. I was none too
pleased, needless to say. I was mostly concerned that I was not going to have
enough time between my surgery consult and the surgery to get everything I need
to get done, done.
With that being said, I still love Dr. S. Two of the three times
he re-scheduled, it was out of his control. I cut him some slack.
I DID have my surgery consult this past Monday, the 20th,
and here is a summary of what I learned:
Overall, Dr. S. is not overly concerned about me using the crutches
or not using the crutches prior to surgery. He said it’s not generally his
protocol, but that I can use them if it makes me more comfortable. He also said
that he doesn’t believe it will make any difference either way on the outcome
of the surgery.
I can (and should) get a handicap plate if I will be more
comfortable afterwards. I will start this process within the next couple weeks.
It’s (apparently) very easy, just a form you fill out and your doctor signs it confirming
the need.
I do not have to do the Autologous blood donation (where you
donate blood to yourself) because Dr. S. uses a machine called an Intraoperative
Cell Salvage Machine, a.k.a. “cell saver.” This may be graphic, but I think it’s
super cool so deal. The machine uses suction to collect the blood I lose during
surgery, it then washes and filters it so it can then be put back into my body.
It’s like a conveyor belt of blood. Science is amazing, isn’t it?
The actual procedure, performed by Dr. S. and a fellow at Rhode Island Hospital, will take approximately 2-3 hours depending on how much work
they do on the labrum while they’re in there. Dr. S. may have his partner from
Texas fly up to accompany him with the surgery, but he’s not sure if he will do
that yet.
Once the surgery is complete, I will be in the hospital about 3-5
days. I will start moving and flexing the joint post-op day 1, but I will be
non-weight bearing for approximately 8-12 weeks. When the bone finally heals completely,
I can start the more rigorous physical therapy and can pretty much go as hard
as I can on it (in terms of PT). I will need to do about 2-3 days a week of PT.
I will be visiting the PT office at least once a week, but I can do the
additional day or 2 at home on my own. I can return to work around 8 weeks
after surgery, depending on my progress. I will be on TDI in the meantime.
After about 6 months, I should be feeling really great. However,
he doesn’t expect me to be completely “normal” (or as close as my crazy self
can get) until about a year after surgery.
The surgery will not influence my ability to carry or deliver a
child, the only stipulation is that I cannot carry a baby until after all of
the bone has healed. That’s really a non-issue for us; we’re not ready to have
kids yet anyway.
Those were all the good things I learned, things that made me
think “maybe this won’t be so bad after all!” There were two issues that came
up during the conversation that had me a bit bothered. The first pertains to
the activity level for me once this surgery is complete. Dr. S. came right out
and told me that patients that undergo this surgery are almost always
instructed that they cannot return to ANY athletic or strenuous activity,
whatsoever, after the surgery. Ever. As
in, never again. That did not sit well with me. I basically told him that he
couldn’t be serious, to which he replied: Patients are only cleared to walk and
MAYBE light bicycling. What the crap? Talk about a blow. He said he knows that
that is not always a realistic plan for people. I told him that there was no
way that I was not ever going to do anything athletic or “strenuous” ever again.
He gave me lots of “Will you please just listen to your surgeon?” looks and
after a few minutes of discussion he said that he would be fine with 1 day a
week of any given activity. So, for instance, I can play volleyball, OR, I can
line dance. I can go for hike, OR, I can do a short jog. I can only do one
thing a week that puts any kind of stress on the joint. Otherwise it’s walking
only. No running, no treadmill (which I hate anyway), no long bike rides, even
swimming is going to be a no-no. LAME. I am unhappy.
However, I keep trying to tell myself that things could be SO
MUCH WORSE. The past few days, over here in New England, the Jimmy Fund has
been having the Jimmy Fund Radio-telethon. They’ve been having TV and radio
interviews with all of these cancer patients whom, I’m sure, would trade places
with me in a heartbeat. It’s unfair and childish for me to complain about
something so trivial when there are people out there with real-for-real health
issues…issues that can’t be fixed with just a few cuts of some bone and a
couple steel pins. I have been extremely blessed with a healthy and outrageously
happy life so far (with a few obvious exceptions). I have a family I wouldn’t
trade for the world and a husband that drives me crazy but I just can’t live
without (hehe ;o) ). I have a wonderful life, so I’m not going to stress over a
little, itty-bitty issue like this.
Moving on. The second thing that bugged me about my consult was
that Dr. S. said he may not fix the labrum while he’s completing the surgery.
He explained that he wants to complete the surgery with as little trauma to the
joint as possible. Considering the surgery already includes a bone saw, I’m
thinking we’re probably going to not be getting the labrum fixed. However, he
did say that he’s gonna “take a peek in the joint,” whatever that means, and
see if it’s an easy fix. He said if it’s something he thinks he can fix easily
and not be an extensive part of the procedure than he’ll go ahead and take the
joint apart to repair the labrum. He also soothed some fears by saying that a
lot of times with patients that have DDH like mine, once you fix the structure
of the joint…the labrum pain subsides and becomes a non-issue. That is another
reason why he’s not sure he wants to take the time to repair it while I’m under
anesthesia, he’d rather have me under for as short of a time as possible.
The surgery is still scheduled for October 26th. I
need to go within 30 days of the procedure to have all of my pre-op bloodwork
completed. This includes a coagulation time test. Um, I’m sorry, what? The
things you’d never even think of.
Also! The day before the surgery the hospital will deliver a
Continuous Passive Motion machine. This ought to be fun. Google that sucker,
tell me if you don’t chuckle. It looks absurd!
“Continuous passive motion (CPM) devices are utilized to keep a
joint in motion without patient assistance. CPM is being evaluated for
treatment and postsurgical rehabilitation of the upper and lower limb joints
and for a variety of musculoskeletal conditions.”
I can’t wait to try this thing, how awkward is that? It moves for
you. I will, most certainly, be posting video of that thing once I’ve got it.
In the meantime, I’ll keep you posted on any and all new info.
Thanks for reading!
D
Friday, July 20, 2012
It's all fun and games until someone sets a date.
Well, we’ve had in interesting couple of months on this hip
journey. Originally, I was supposed to have my surgery consult back in
mid-June. It was cancelled because Dr. S wanted to see me on a day when he had
no other patients. We then scheduled it for July 16th. So, this past
Monday, my hubby and I mentally prepared ourselves for the big meeting. We
gathered all of our questions, looked at dates on a calendar, and prepared
ourselves to learn all we needed to know about, and schedule my surgery in the
fall.
We arrived at the hospital only to find out that Dr. S had been
called to an emergency surgery and he would not be able to see us. What a huge
bummer. It took a lot of effort to not be selfish about it, and not be
aggravated that we weren’t even notified (turns out we were…which is a whole
other story in and of itself). I just tried to remember that if it were me that
needed emergency surgery, I’d want Dr. S to drop everything for me, too. I will
admit that I was more nervous and emotionally invested in this appointment than I
had thought. I was pretty deflated the rest of the day.
My biggest concern
leaving the hospital that day is that if we waited much longer to schedule than
we wouldn’t be able to get the time-frame that we wanted. I would be upset
knowing that I had been waiting for MONTHS to schedule the surgery and in the
end we couldn’t get the time I wanted. So, when I called Dr. S’s wonderful
assistant, I explained my worries. She completely understood and said that we
would schedule my date right then and there! Who knew it would be so easy. So,
the date of the PAO is officially set for October 26, 2012. I will have my
surgery consult on August 6th (hopefully).
So, we are just over three months away from surgery! That is just
mind-boggling. It’s a strangely wonderful feeling to have an actual date to
look forward to (or dread, however you want to put it), but it’s also very
scary to now know that it is, indeed, going to happen. All of a sudden, it’s
very finite. I actually AM going to have surgery and it WILL be before the end
of the year. Yikes. I keep waiting for someone to call up and say “Just
kidding! Your images look fine, it’s just a little something-something with an
easy fix.”
You see, before it was so fluid. I’m going to have surgery eventually. I’m going to have surgery to
fix my hip “down the road.” I
remember the original appointment with Dr. E from 10 years ago like it was
YESTERDAY. I distinctly remember him saying: “You’re going to need surgery by
25-30.” I remember thinking he was loon (among other things), I would never
need surgery. And here I am! Where the heck did that time go? And since when do
we age so quickly, both in years, and in condition? It’s been 10 years…and it
feels like it’s been the blink of an eye.
I refuse to get philosophical…so I will leave with this:
I have my consult on August 6th. I believe this will
be the first truly informative appointment, which will lead to the first truly
informative entry.
Questions for Dr. S include but are not limited to:
Am I given a list of things to do beforehand?
Should I get a temporary handicap plate?
I have heard of people donating blood to themselves beforehand
for this surgery, should I?
Who will be performing the surgery with him?
How long is the surgery?
How long should I stay out of work on TDI?
How long after surgery should we wait to have kids?
I’ll be sure to post as soon after the surgery consult as I can.
Hopefully it actually happens this time!
Thanks for listening/reading/following my journey,
D
Wednesday, May 23, 2012
Everyone needs a crutch.
Everyone needs a crutch…quite literally in my case.
This past weekend was my first weekend “on crutches.” At my
appointment with Dr. Kim on May 4th, he suggested that I start using
crutches when I do any significant amount of walking. When he first said this
to me…I was taken aback and actually pretty upset. He says that using the
crutches, or a cane for short distances, will help me get used to using them for when I need them all the time after the surgery (post-surgery I will be non-weight bearing for 3-6
months). Dr. K also said using these will help me to reduce fatigue in the
joint and allow the inflammation in my labrum to subside. Dr. K said he wants
me to be completely pain free going into the surgery in the fall.
Listen, I get it…a lot of people have serious injuries that are
a lot worse than mine…life-changing injuries/deformities that don’t allow them
to ever walk the same, or ever walk again, period. So, please don’t take this
the wrong way. I’m not saying this is HORRIBLE or the worst thing that could ever
happen. But it IS happening…and it IS a prohibitive deformity.
Here’s the thing…I
am the definition of a DO-ER. I can’t sit still for five minutes. I work 40+
hours a week, I play volleyball at least once, sometimes twice a week, I
Co-Chair the local Relay For Life and on Sunday’s I volunteer at the local zoo. My husband and I are lucky if we get to spend one night a week together. But
that’s how I am…I thrive on being busy. I’m also proud and very stubborn.
This is now the first time where I really HAVE to slow down
because of my hip. It’s my first real speed bump. Playing less volleyball was
bothersome, but I can deal with it because I still can play sometimes. Not
wearing high heels anymore doesn’t really bother me because I didn’t like them
in the first place. And I’ve been walking with a limp for so long that I don’t
even realize I do it anymore. But walking with crutches is a bit (here’s that
word again) discouraging. It’s cumbersome, and awkward. People stare at you,
they pity you, and worse, they go out of their way to help you. It’s a bit of a
blow to the ego and the pride. It’s embarrassing. I know people are just being
nice, (and honestly, thank GOD they hold the door for me because I really don’t
know how I’d get it if they didn’t) but it’s discouraging to know that the person
holding the door, or letting me cut them in line, is doing it because they feel
bad for me.
And when I use the cane it’s even WORSE. Kids stop dead in their
tracks and stare at me. They ask their parents “How come she has that?” and “What’s
wrong with her?” Awesome. I know they don’t know any better, I’m not upset with
the kids…it’s just that this whole thing is going to be a serious adjustment.
And it’s only just beginning.
With all of that being said…and I hate to admit this…the freaking
things help me so much. My hip felt glorious
after the whole day of being on the crutches. At the end of the day on
Saturday, my husband gave me the “I told you so” look, which is my least
favorite look in the whole wide world, especially from him. Saturday morning, just
thinking of everything we needed to do made my hip hurt. Our schedule on
Saturday consisted of the following: Out for breakfast, Anne and Hope, a Target
trip, Harbor Freight Tools, Christmas Tree Shop, and Lowes. The amount of
walking we did at Anne and Hope, on a normal day, would have benched me for the rest of the
day, walking wise. However, I did ALL of that…and then I went home and planted
14 flower pots and 4 window boxes! I felt GREAT. And just for comparison: I
worked at the zoo the next day and an hour into my shift I was limping and
having a hard time.
I think my biggest mental roadblock, when it comes to the
crutches, is that I've spent so much of my life telling myself that nothing's
wrong and that I can just continue to go about my business like there's no issue. Just something I can continue on with, and it's no big deal. Even with the pain, I was okay with that because I didn't have to admit
that I have any kind of disability, or problem. This is really the first time
that I feel like what I have going on really IS a big deal. It's hard to come
to terms with something like this when you've spent so much of your time trying
to tell yourself it's nothing. I hate complaining about something as silly as
using crutches, but deep down it’s NOT the crutches I’m upset about, it’s the
fact that this really is happening…and that I really do need to face this
issue. It’s the “What’s wrong?” questions, the “Why are you using a cane?”
questions that bother me…because then I dive into the whole ordeal instead of
just ignoring it.
So, I’m
starting to come to terms with everything, and in the grand scheme of things I
know that I am lucky that this is all that I have. I could have serious,
life-threatening issues. I’m lucky to be happy and healthy with a good family
who loves me. However, after this weekend, it’s becoming more and more clear to
me that this is whole journey is going to be more complicated than I thought…emotionally
and physically.
Saturday, May 5, 2012
Whad'dya need ta know about PAO?
Hello, again!,
I went to Massachusetts General Hospital yesterday and met with
Dr. Kim for a second opinion on my DDH. In short…he told me that Dr. Schiller’s
recommendations were correct. That I absolutely do need PAO, and the sooner I
get it, the better.
Dr. K gave me some great information. He explained to me that PAO
is one of the rare circumstances that they suggest you go through with the
surgery BEFORE you are experiencing any hip pain at all (currently, all of the
pain I feel is from the tears in my hip labrum), that is because the philosophy
with this type of deformity is that you “go into surgery without pain, come out
without pain.” Essentially, if you’re already having joint pain before you have
anything done, chances are you’re going to come out of the surgery with pain,
the damage has already been done.
I came out of there feeling like this is definitely something
that I do HAVE to have done, and that it is the right incision…I mean decision
(see what I did there? Gotta keep the mood light).
I thought that this would be a good time to show you exactly what
is wrong with my hip, and how they are going to fix it. I’m going to attach my
actual medical imaging, and try and compare it to my normal hip so you can
see what is going on. I’ll then explain to you, in as much detail as I have,
what Dr. S will be doing to fix my hip deformity.
So,
first off, here is a series of imaging of my hip. I’ll try to explain what they
are as I show them.
This is an x-ray of both hips. It shows a mostly normal left hip, and my sad right hip.
To the left is an image in a 3D CT Scan of my right hip. This view is posterior, or from the back. Here you can see what is the proper coverage of the femoral head.
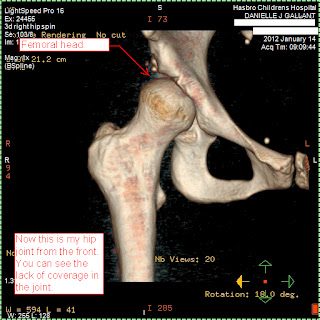
Now, this is the front of my hip socket. You can see how much coverage I'm lacking on both the top of the femoral head and also in front. I have less than 45-50% coverage.
This one is just an extra view from the 3D CT Scan, which blew my mind. This is looking from INSIDE my pelvis, out towards the joint. See how I've got pretty good coverage in the back part of the joint, but the front part of the joint is really crappy looking.
The opposite angle from above. Mostly I posted these because I think they are crazy. The imaging that they can do today boggles my mind!
Additionally, I have labral tears in my joint. This is really common in DDH patients. But the MRI is awesome, so I thought I'd post it. This picture is if you're looking from the top looking down, into the hip joint. The circle in the middle is my femoral head.
How do you fix this? Well, obviously PAO. So, I've inserted some information from a really great website who describes in regular people language...instead of doctor-speak.
-Hip Preservation Surgery for Adult Hip Dysplasia"This surgery involves cutting the pelvis around the hip joint and shifting it into a better position to support the stresses of walking (OR volleyball...okay the website didn't say this...but I did!). After the hip is re-positioned, it is held in place with screws until the bone heals. After the bone heals, the screws can be removed, but this is not usually necessary."
http://www.hipdysplasia.org/Content.aspx?id=9252
That makes it sound sooooo easy, doesn't it? They also had these neat looking little diagrams:
So, that is that! It's looking like I will be having the surgery sometime this fall. Probably October/November. In the meantime, Dr. Kim suggested yesterday that I start using crutches when I can to try and get my pain under control. The idea is to reduce usage which will reduce inflammation in my labrum, therefore reducing my pain. He said the best condition to be in when going into the surgery is to go in without any pain. While I'm under for the PAO, they will also be attempting to fix the labral tears. It will depend on what they find when they get in there.
From here, I'll post as I learn new things and go through the process of getting ready for surgery.
Thanks for reading! Please feel free to post any questions you have and I'll try to answer them as best that I can.
Your gimpy friend,
Danielle
Subscribe to:
Posts (Atom)